Insulin is a hormone produced by the beta cells in the pancreas. It facilitates the uptake of glucose from the bloodstream into the cells, where it is used for energy or stored for future use. Without adequate insulin, blood sugar levels can rise to dangerous levels, leading to a variety of health complications.
Types of Diabetes and Insulin Needs
There are two main types of diabetes, each with different insulin requirements:
- Type 1 Diabetes: This is an autoimmune condition where the body’s immune system attacks and destroys the insulin-producing beta cells in the pancreas. As a result, individuals with Type 1 diabetes produce little to no insulin and require external insulin administration for survival.
- Type 2 Diabetes: This type is characterized by insulin resistance, where the body’s cells do not respond effectively to insulin. Over time, the pancreas cannot produce enough insulin to maintain normal blood sugar levels. While lifestyle changes and oral medications are often first-line treatments, many people with Type 2 diabetes eventually require insulin therapy to manage their condition effectively.
Types of Insulin
There are several types of insulin used in diabetes management, each varying in how quickly they begin to work and how long they last:
- Rapid-Acting Insulin: Begins to work within 15 minutes and lasts for 2-4 hours. It is often taken just before or after meals to control blood sugar spikes.
- Short-Acting Insulin: Takes effect within 30 minutes and lasts 3-6 hours. It is typically used to cover insulin needs at mealtimes.
- Intermediate-Acting Insulin: Starts to work within 2-4 hours and lasts up to 12-18 hours. It is often used in combination with short- or rapid-acting insulin.
- Long-Acting Insulin: Provides a steady insulin level that lasts for up to 24 hours. It is usually taken once or twice a day to maintain baseline insulin levels.
- Ultra Long-Acting Insulin: Can last more than 24 hours and is designed to provide a stable, long-term insulin effect with minimal peaks.
Methods of Insulin Delivery
Insulin can be administered in various ways depending on individual needs and preferences:
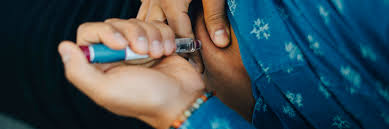
- Syringes and Pens: Traditional methods where insulin is injected subcutaneously. Pens offer more convenience and precise dosing compared to syringes.
- Insulin Pumps: These devices provide continuous insulin delivery through a catheter placed under the skin. Pumps offer more flexible and precise insulin management, especially useful for those with Type 1 diabetes.
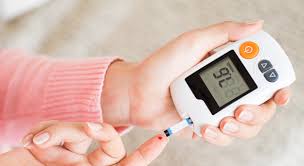
- Continuous Glucose Monitors (CGMs): While CGMs do not deliver insulin, they provide real-time blood sugar readings that help individuals adjust their insulin doses more accurately.
Benefits of Insulin Therapy
Insulin therapy can significantly improve blood sugar control and reduce the risk of diabetes-related complications. Proper use of insulin helps:
- Maintain Blood Sugar Levels: Keeping blood sugar levels within target ranges reduces the risk of complications such as heart disease, kidney damage, and nerve damage.
- Enhance Quality of Life: Effective insulin management allows individuals to maintain more normal blood sugar levels, improving overall health and energy levels.
- Prevent Diabetic Ketoacidosis (DKA): For those with Type 1 diabetes, insulin is essential in preventing DKA, a serious condition caused by extremely high blood sugar and ketone levels.
Challenges of Insulin Therapy
Despite its benefits, insulin therapy can be challenging. Some common issues include:
- Hypoglycemia: Low blood sugar can occur if too much insulin is administered or if meals are skipped. It’s important to monitor blood sugar levels regularly.
- Weight Gain: Insulin therapy can sometimes lead to weight gain, necessitating careful dietary and lifestyle management.
- Injection Site Issues: Repeated insulin injections can cause lipodystrophy, where fat tissue breaks down or builds up, affecting insulin absorption.
Future of Insulin Therapy
Advancements in insulin therapy continue to improve diabetes management. Innovations such as:
- Artificial Pancreas Systems: These combine CGMs and insulin pumps to automate insulin delivery, closely mimicking natural insulin production.
- Faster-Acting Insulins: New formulations that act more quickly and predictably are in development.
- Non-Invasive Delivery Methods: Research is ongoing into methods such as inhalable insulin to improve convenience and adherence.
Insulin is a crucial component in the management of diabetes, enabling individuals to maintain healthy blood sugar levels and reduce the risk of complications. While it requires careful management and monitoring, the benefits of insulin therapy far outweigh the challenges, contributing to a better quality of life for those living with diabetes